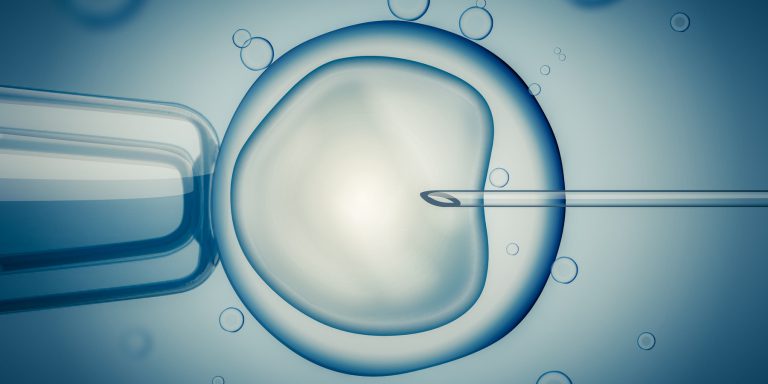
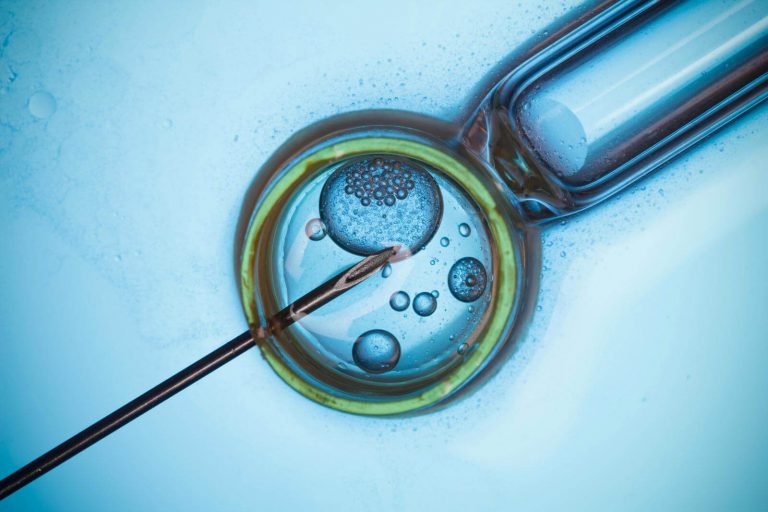
An endometrial receptivity array (ERA) is a type of test used on women going through IVF to determine the optimal timing for embryo implantation. It is primarily used for cases of repeated implantation failure following embryo transfer.
What is Embryo Implantation?
After sperm fertilizes an egg to form an embryo, that embryo moves from the fallopian tubes to the uterus where it implants into the endometrium, or uterine lining.
If IVF is used, then the embryo is formed in the lab rather than in the fallopian tubes. Implantation will happen after embryo transfer, when the embryo is put directly into the uterus.
To prepare for pregnancy, the endometrial lining in the uterus thickens and becomes receptive to implantation of a fertilized egg. This happens in response to hormone secretion, with estrogen and progesterone being the primary hormones that are released to ensure the endometrial lining is receptive to pregnancy. The external cells of the embryo and the uterine inner lining, together, will create the future placenta.
What Causes IVF Implantation Failure?
When conceiving naturally, implantation may fail due to a lack of estrogen leading to a thin uterine lining. Additionally, problems with the lining, such as scarring from previous infections can affect implantation.
Even when the body produces the right hormones to thicken the endometrial lining, it happens on a tight schedule according to an internal clock that the body expects the embryo will implant. This “window of implantation” (WOI) typically starts on day 19 or 20 of a menstrual cycle and may be “open” for 4-5 days.
The entire process is extremely complex and involves the careful alignment of various biochemical, morphological and genetic factors. The process of implantation is further complicated by the fact that the egg and the uterine lining need to essentially communicate with each other when they are ready.
In IVF, a woman will typically receive progesterone and estrogen in order to assist the thickening process. IVF failures may be due to poor timing of progesterone administration and how that is coordinated with the WOI. The failure can also occur when a woman’s WOI does not follow the typical schedule, which can begin earlier or later than the average “19 or 20th day” of a menstrual cycle.
When is an ERA Used?
An estimated 25% of patients with recurrent failed embryo transfers experience a lack of coordination in this process, leading to IVF failure. The ERA has been developed as a means of identifying this window more accurately in order to improve chances of pregnancy for those undergoing IVF.
Typically the test is recommended after repeated implantation failures, or if there is other reason to be concerned about thin uterine lining. Assessing the lining with the ERA test allows for fertility doctors to pinpoint the best day for the embryo transfer procedure.
How Much Does an Endometrial Receptivity Array Cost?
The cost of an ERA is around $850, which in addition to the costs of fertility medication and medical visits can be significant for most.
The additional cost and time required is one prohibitive factor for why the test is not used up front in more IVF cycles. However, some patients should consider pursuing more testing like the ERA up front. This additional expense can be the difference between one successfully timed IVF cycle and multiple failed cycles.
How Does an ERA Work?
The ERA is a tissue test which evaluates the receptivity of the endometrial lining to determine the optimal timing for pregnancy, or the “window of implantation”. It is performed based on the assumed WOI for a woman during a natural cycle or an HRT (hormone replacement therapy) cycle.
The test consists of an endometrial biopsy, where a small painless sample of the tissue is collected and analyzed genetically to determine the optimal timing for hormone administration and implantation in the current or subsequent round of IVF. Usually, most the protocol is to transfer the embryo at day-5 of growth, however, for about 25% of women that estimate is not accurate–some may need the embryo transfer to occur earlier or later, and that’s where the ERA test can be beneficial.
The test results are either “receptive” or “non-receptive”. If they are non-receptive, a second ERA test will usually be required in order to determine the WOI. However, if they are receptive, this may allow the embryo transfer to be transferred on that same day for the best success. If embryo transfer is to proceed in the following month, it will happen on that day but one month later. This gives fertility doctors the opportunity to thaw and prepare eggs or embryos so that they are ready to be implanted in the uterus in the following month.
Although the ERA test is an additional expense, for some 25% of patients it might be useful to know the optimal time for embryo transfer as a means to avoid additional IVF procedures. Speak with your physician to determine if the ERA test is right for you.