We’ve all heard the simple tales about the birds and the bees. But for those trying to conceive who want a little more detail about how babies are made, you’ve come to the right place. In order to create a successful pregnancy, several distinct stages of embryo development have to occur. A sperm must reach, penetrate, and fertilize an egg to form a zygote. The zygote must divide and form a blastocyst. The blastocyst must reach the uterus and implant in the endometrium. The implanted blastocyst continues its development into an embryo and then a fetus.
In this guide, we will explain each of these crucial stages and offer insights about what’s going on in your body as you explore the path to parenthood.
1. Fertilization
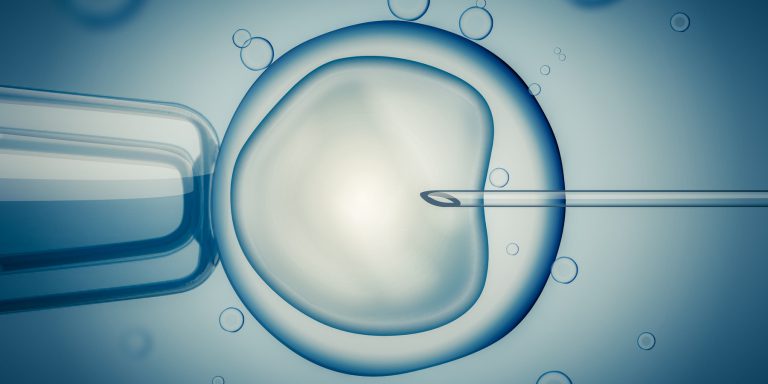
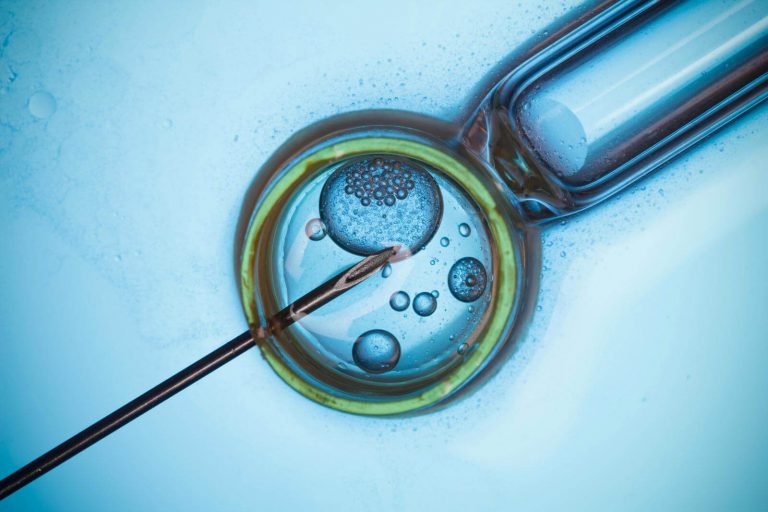
Fertilization is the union of the female gamete (egg) and the male gamete (spermatozoa). Whether it occurs naturally inside the female reproductive system or with the assistance of reproductive technologies outside of the human body, the product is a structure called a zygote.
When a female is ovulating, she releases one egg into her Fallopian tubes (or more in the case of fraternal twins). During this time, a female’s cervical mucus will thin, in preparation for sperm to pass through more effectively.
Following spermatozoa ejaculation inside the vagina, special secretions help them to swim through the cervix towards the uterine tube where fertilization takes place when the sperm penetrates the egg within 24-72 hours.
The fertilized egg, or zygote, then begins to move toward the uterus. This cluster of cells rapidly divides, forming an embryo within a complex structure known as the blastocyst.
What can prevent fertilization?
There are a wide range of reasons why fertilization may not occur, but they all have the same outcome. Something is stopping sperm and egg from reaching each other.
Absence of Sperm/Egg: If a female has an anovulatory cycle where she doesn’t release an egg, or if no sperm reaches the egg because of azoospermia or low sperm count, then fertilization will not occur.
Sperm’s Ability to Reach the Egg: Poor sperm motility or movement, or poor chemotaxis (sperm’s ability to navigate toward the egg) can prevent fertilization. Similarly, if a female’s cervical mucus does not thin enough during ovulation, sperm may not be able to reach the egg.
Sperm Penetration: Poor morphology, or abnormal sperm shape, can make it harder for sperm to penetrate an egg. Sperm also relies on a chemical reaction, called an acrosome reaction, that helps it create a hole in the egg to pass through. Poor or incomplete acrosome reaction could also inhibit fertilization.
Sperm Quality Testing. Easy, Mail-in Kit.
ORDER NOW2. Blastocyst Development
This blastocyst structure comprises two sets of cells—inner and outer cells—along with fluids. Throughout its maturation, the blastocyst is encased in a protective layer called the zona pellucida, similar to an eggshell. The outer cells beneath this covering play a crucial role in developing the future placenta and surrounding tissues, essential for supporting fetal growth within the uterus. Meanwhile, the inner cells of the blastocyst will eventually differentiate into various tissues and organs, such as bones, muscles, skin, liver, and heart.
The cells within the blastocyst undergo rapid growth, experiencing numerous transformations as they specialize, resulting in a tightly structured form. In humans, these dynamic changes occur in the initial days of development, preceding the implantation phase in the uterus. During this stage, the zona pellucida, or the eggshell, eventually breaks, freeing the blastocyst. It then traverses the Fallopian tubes, journeying towards the uterus where it successfully implants around the tenth day.
What can prevent blastocyst development?
Blastocyst arrest is the term for when the cells fail to divide, stopping the developmental progress of the embryo. While the exact causes of blastocyst arrest are not fully understood, they are typically related to genetic abnormalities in the sperm or egg.
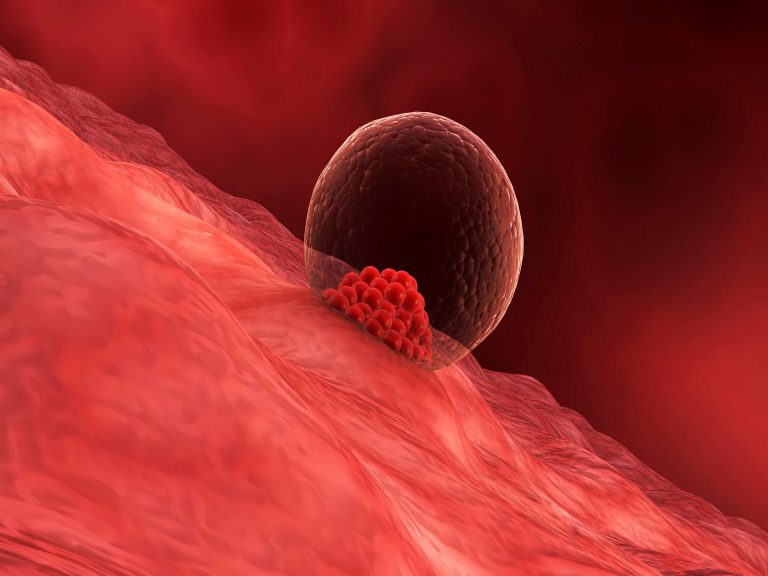
3. Blastocyst Implantation
When the blastocyst reaches the uterus, it implants in the endometrium–the mucus membrane which lines the uterus. The external cells of the blastocyst and the uterine inner lining, together, will create the future placenta. The placenta is a structure that transfers nutrients to the baby and removes its wastes.
What can prevent implantation?
Sometimes, a blastocyst will not implant in the uterus. Scientific evidence suggests that the endometrium plays a crucial role in the selection of the blastocyst before facilitating implantation. This mechanism eventually results in the implantation of healthy blastocysts or the rejection of abnormal blastocysts. Some human blastocysts have alterations in their genes that can delay or obstruct normal development. If such blastocysts do implant, there is a higher risk of miscarriage due to the genetic abnormalities.
When a fertilized egg is able to implant in the uterus but fails to develop, it is described as an empty gestational sac, or “blighted ovum”. This may also occur due to the presence of abnormalities in the chromosomes of the sperm, the egg, or the fertilized egg. This typically happens in the early days of pregnancy.
4. Embryo Development
As the blastocyst reaches the final steps in the implantation process into the inner lining of the uterus, it evolves into a structure called an embryo. At this point, internal organs and external structures begin to develop. The mouth, lower jaw, throat are emerging, while the blood circulation system starts its evolution and a heart is created. The ears arise, and arms, legs, fingers, toes, and eyes are being shaped. The brain and the spinal cord are already formed, while the digestive tract and sensory organs start their development. The first bones are replacing the cartilage.
After ten-twelve weeks of pregnancy, the embryo moves into the final stage of development–a fetus.
What can prevent embryo development?
With so many internal organ systems and external structures beginning specialization and development in the embryo, the developing organism is particularly sensitive to damage from genetic abnormalities and environmental exposures. These genetic abnormalities can range from spontaneous genetic mutations to improper chromosome arrangement that can potentially affect the development of important structures like the heart or brain.
Alongside genetic abnormalities, any number of environmental factors (malnutrition, infections, disease, toxic exposures) can have an effect on genetic expression potentially proving to be lethal to the developing embryo.
Issues with embryonic development can occur as early as the first three weeks.
5. Fetal Development
By the twelfth week of fertilization, the embryo moves into the final stage of development, known as the fetal stage. By now, the fetus has formed all of the organs and structures necessary for a baby, but those organs still need to grow and develop.
At three months of pregnancy, the upper and lower extremities of the fetus are completely developed. Ears and teeth are formed and the reproductive organs have evolved. At the end of this month, the fetus has completed the expansion of most of the circulatory and urinary systems. It’s about the size of a plum or a lemon.
At six months, the fetus can respond to sounds. The fetus continues to develop and grow changing position and responding to sounds and other stimuli. Its body is around the length of a large ear of corn.
By eight months, the brain is evolving quickly so the baby can see and hear, although the respiratory system requires maturation. The baby is now about the size of a butternut squash or a pineapple.
At nine months, the baby starts responding to stimuli and can move its entire body–which is about the size of a watermelon. However, the limited space around the growing human becomes increasingly cramped. When the baby has not yet changed its position inside the uterus, this marks the appropriate time for it to descend into the pelvis, preparing to enter the birth canal and face the world.
What can prevent fetal development?
Because all major structures are already formed in the fetus, the fetus is not as sensitive as the embryo to damage from environmental exposures. This is why after the first trimester, a miscarriage is much less likely. However, toxic environmental exposures can still contribute to physiological abnormalities or minor congenital malformations.
The Importance of Fertility Testing for Successful Embryo Development
Each of the above steps are crucial in the path to pregnancy. To that end, fertility testing can be a pivotal tool that offers valuable insights into the underlying factors that can influence each of these stages. By undergoing fertility testing, couples can gain a comprehensive understanding of their reproductive health and be better equipped to navigate potential challenges. From assessing sperm quality to understanding potential genetic factors, fertility testing serves as a pragmatic guide, allowing couples to optimize their chances of a successful pregnancy. In the realm of conception, knowledge is power, and fertility testing empowers couples to embark on their path to parenthood with confidence and preparedness.
Sources:
- Ngwenya, J. B. https://embryology.med.unsw.edu.au/embryology/index.php/Fertilization#Oogenesis. (Paper Bag Publishing, 2009).
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3521485/
- https://www.reproduction-online.org/content/142/6/759.full
- https://study.com/academy/lesson/what-is-a-blastocyst-definition-development-stages.html. Available at: https://study.com/academy/lesson/what-is-a-blastocyst-definition-development-stages.html. (Accessed: 6th June 2017)
- https://embryology.med.unsw.edu.au/embryology/index.php/Blastocyst_Development#Introduction. Available at: https://www.mendeley.com/library/. (Accessed: 6th June 2017)
- https://www.medicinenet.com/script/main/art.asp?articlekey=18258. Available at: https://www.medicinenet.com/script/main/art.asp?articlekey=18258. (Accessed: 6th June 2017)
- Blighted ovum: What causes it? – Mayo Clinic. Available at: https://www.mayoclinic.org/diseases-conditions/pregnancy-loss-miscarriage/expert-answers/blighted-ovum/faq-20057783. (Accessed: 6th June 2017)
- Brosens, J. J. et al. Uterine Selection of Human Embryos at Implantation. Sci. Rep. 4, 3894 (2015).
- Fetal development week by week – BabyCentre. Available at: https://www.babycentre.co.uk/pregnancy-week-by-week. (Accessed: 6th June 2017)